Male sterilisation, commonly known as a vasectomy, is a safe and highly effective method of permanent contraception. Many men consider this option once their family is complete or when long-term contraception is preferred. However, despite how common the procedure is, questions about the vasectomy procedure and recovery are entirely normal.
This article explains what a vasectomy involves, how the procedure is performed, what recovery looks like, and answers the most frequently asked questions. The aim is to provide clear, evidence-based information in a straightforward and professional manner.
What Is a Vasectomy?
A vasectomy is a minor surgical procedure that prevents sperm from entering the semen. During ejaculation, semen is still produced as normal, but it no longer contains sperm. As a result, fertilisation cannot occur.
The procedure works by sealing or dividing the vas deferens, the tubes that carry sperm from the testicles to the urethra. Because the body continues to produce sperm, they are naturally reabsorbed.
Importantly, a vasectomy does not affect testosterone levels, sexual performance, erections, or libido.
Further Reading: https://www.nhs.uk/contraception/methods-of-contraception/vasectomy-male-sterilisation/what-is-it/
Advantages of Vasectomy
- Highly effective
- Permanent
- Simple procedure
- Short recovery
- No ongoing contraception required once confirmed
Disadvantages to Consider
- Permanent decision
- Minor surgical risks
- Need for follow-up testing
- Rare risk of chronic discomfort
Who Is a Vasectomy Suitable For?
A vasectomy is suitable for men who:
- Are certain they do not wish to father children in the future
- Have completed their family
- Want a reliable, long-term contraceptive option
- Prefer a permanent alternative to female sterilisation
Although vasectomy reversal procedures exist, they are complex and not always successful. Therefore, a vasectomy should always be considered permanent.
How Effective Is a Vasectomy?
A vasectomy is more than 99% effective once post-procedure semen testing confirms the absence of sperm. It is one of the most reliable forms of contraception available.
However, it is important to understand that contraception is not immediate. Sperm may remain in the tubes for several weeks following the procedure. This is why follow-up testing is essential before stopping other contraceptive methods.
The Vasectomy Procedure Explained
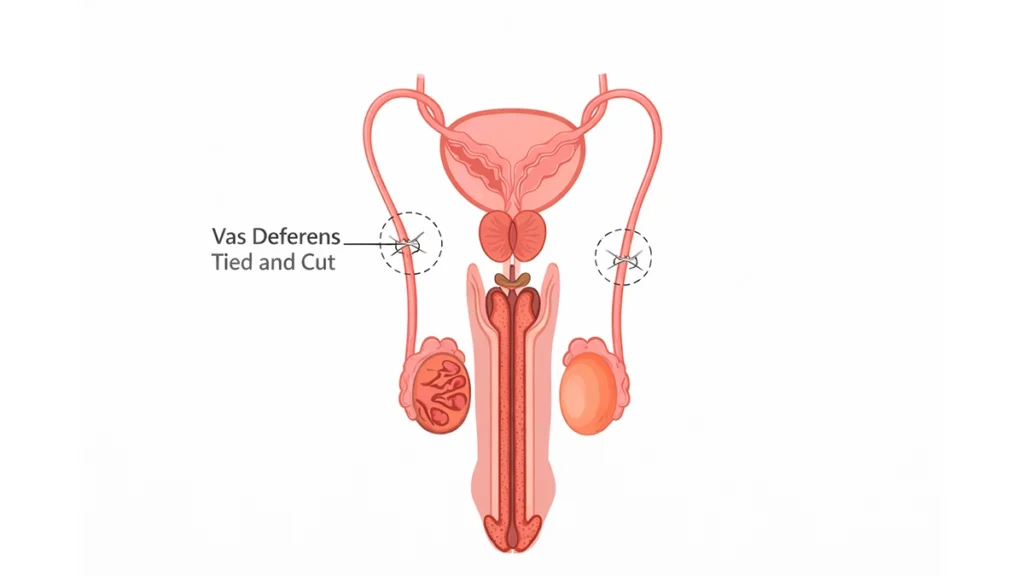
Understanding the vasectomy procedure and recovery helps reduce anxiety and allows men to prepare appropriately.
Before the Procedure
A consultation takes place beforehand to:
- Confirm suitability
- Discuss risks and benefits
- Explain alternatives
- Answer questions
During this appointment, informed consent is obtained, and patients are encouraged to raise any concerns.
How the Procedure Is Performed
A vasectomy is usually performed under local anaesthetic and takes approximately 20–30 minutes.
There are two main techniques:
1. Conventional Vasectomy
A small incision is made in the scrotum. The vas deferens are identified, divided, and sealed. The incision is then closed.
2. No-Scalpel Vasectomy
A small puncture is made rather than a traditional incision. The tubes are gently brought to the surface, divided, and sealed. This method typically results in:
- Less bleeding
- Smaller wound
- Faster recovery
Both techniques are safe and effective. The choice depends on the surgeon’s preference and clinical circumstances.
What Happens During the Procedure?
- The scrotal skin is cleaned.
- Local anaesthetic is administered.
- The vas deferens are isolated.
- Each tube is divided and sealed (often using cautery or clips).
- The wound is closed if necessary.
Patients remain awake but should not feel pain. Some pressure or mild discomfort may occur.
Most men return home shortly after the procedure is completed.
Vasectomy Procedure and Recovery: What to Expect
Recovery is usually straightforward. However, understanding what is normal is important.
Immediately After the Procedure
It is common to experience:
- Mild discomfort or aching
- Swelling
- Bruising
- A small amount of blood staining on dressings
These symptoms typically settle within a few days.
Patients are advised to:
- Rest for 24–48 hours
- Wear supportive underwear
- Apply ice packs intermittently
- Avoid strenuous activity
Returning to Normal Activities
Most men:
- Return to desk-based work within 2–3 days
- Resume light exercise after about one week
- Avoid heavy lifting for 1–2 weeks
Sexual activity can usually resume after about one week, provided discomfort has settled.
However, contraception must continue until semen analysis confirms sterility.
Further Reading: https://www.nhs.uk/contraception/methods-of-contraception/vasectomy-male-sterilisation/recovery/
Have Any Questions About Vasectomy?
If you are considering male sterilisation or would like personalised advice, a consultation allows for discussion of suitability, risks, and expected outcomes. A thorough assessment ensures you make an informed decision based on your individual circumstances.
Post-Vasectomy Semen Testing
A key part of the vasectomy procedure and recovery process is follow-up semen testing.
Typically:
- Two semen samples are required following a vasectomy. These samples are typically collected at approximately 16 weeks and again at around 20 weeks after the procedure.
- The sample is examined for the presence of sperm
Contraception should only stop once medical confirmation is given that no sperm are present.
Failure to attend follow-up testing can lead to unintended pregnancy.
Risks and Complications
A vasectomy is generally safe, but like any surgical procedure, it carries potential risks.
Common (Usually Minor) Risks
- Bruising
- Mild bleeding
- Swelling
- Temporary discomfort
Less Common Risks
- Infection
- Haematoma (collection of blood)
- Sperm granuloma (small inflammatory lump)
- Persistent testicular discomfort
Chronic pain following vasectomy is rare but can occur in a small percentage of men.
Serious complications are uncommon.
Does a Vasectomy Affect Sexual Function?
A common concern relates to sexual performance.
A vasectomy:
- Does not affect erections
- Does not reduce testosterone
- Does not reduce libido
- Does not alter orgasm
The volume of semen remains almost unchanged because sperm account for only a small proportion of the ejaculate.
In fact, some men report improved sexual confidence because anxiety about unintended pregnancy is removed.
When to Seek Medical Advice After a Vasectomy
During the vasectomy procedure and recovery, medical advice should be sought if:
- Severe pain develops
- Swelling rapidly increases
- Fever occurs
- Persistent bleeding continues
- Signs of infection appear
Early assessment ensures prompt management.
Emotional Considerations

Although vasectomy is physically straightforward, the psychological impact should not be underestimated.
Men should:
- Feel confident about their decision
- Discuss it openly with their partner
- Consider long-term implications
A vasectomy should never be undertaken under pressure.
Frequently Asked Questions (FAQs)
Vasectomy vs Female Sterilisation
Vasectomy is generally:
- Simpler
- Less invasive
- Performed under local anaesthetic
- Associated with fewer risks
For couples considering permanent contraception, vasectomy is often the safer option.
Key Differences Between Vasectomy and Female Sterilisation
| Vasectomy | Female Sterilisation |
|---|---|
| Performed under local anaesthetic | Requires general anaesthetic |
| 20–30 minute outpatient procedure | More invasive keyhole surgery |
| Small scrotal incision or puncture | Abdominal incisions |
| Lower complication rate | Higher surgical risk |
| Short recovery (a few days) | Longer recovery (1–2 weeks or more) |
| Very low risk of serious complications | Small but higher risk of surgical complications |
Summary: Understanding the Vasectomy Procedure and Recovery
The vasectomy procedure and recovery process is typically straightforward. The operation is brief, recovery is usually quick, and complications are uncommon. However, the decision must be made carefully, as vasectomy is considered permanent.
Men who are confident they do not wish to father children in the future may find vasectomy to be a reliable and effective solution.
This content is for general information only and should not be used as a substitute for personalised medical advice. Please speak to a qualified healthcare professional.
Have Any Questions About Vasectomy?
If you are considering male sterilisation or would like personalised advice, a consultation allows for discussion of suitability, risks, and expected outcomes. A thorough assessment ensures you make an informed decision based on your individual circumstances.

